
Get full access with a free account
Benefits of the Coloplast® Professional Educational platform
- Get full access to all educational content, events and resources
- Track your progress
- Share content with your collegues
- Share supporting material with your patient
Take a shorter way to wound healing
By following the steps in this pathway, you can provide an optimal healing environment for malignant wounds and reduce the risk of complications that could lead to delayed healing or worse.
Any advice included here needs to work in conjunction with your local protocols and your individual scope of practice.
This article is based on the book A pathway for treating a person with a: Malignant wound.
What is a malignant wound and what does it look like?
Malignant wounds are predominantly cancer related, however, people at the end of life may present with malignant fungating wounds that are noncancerous in origin.1 Malignant wounds are challenging because of their typical characteristics – excessive leakage/exudate, bleeding, pain, malodour and disfigurement.2 Malignant wounds are also referred to as tumour necrosis, a fungating wound, ulcerating cancerous wound, malignant cutaneous wound, fungating wound, marjolin’s ulcers or malignant lesions. Malignant wounds are often end-of-life wounds that have a low potential for healing, making them challenging to treat and requiring a focus on symptomatic care, with the aim to improve quality of life (QoL).1
This pathway is focused on treating a person with a non-healing malignant wound. Patients with malignancy who have a wound of another ethiology should be treated using the pathway that best matches the wound’s originating ethiology. For example, for a patient with a surgical wound where a malignant tumour has been surgically removed please follow the Surgical Wounds Pathway or if a patient has a venous leg ulcer that turns malignant, but is deemed healable, it is best to follow the Venous Leg Ulcer (VLU) Pathway.
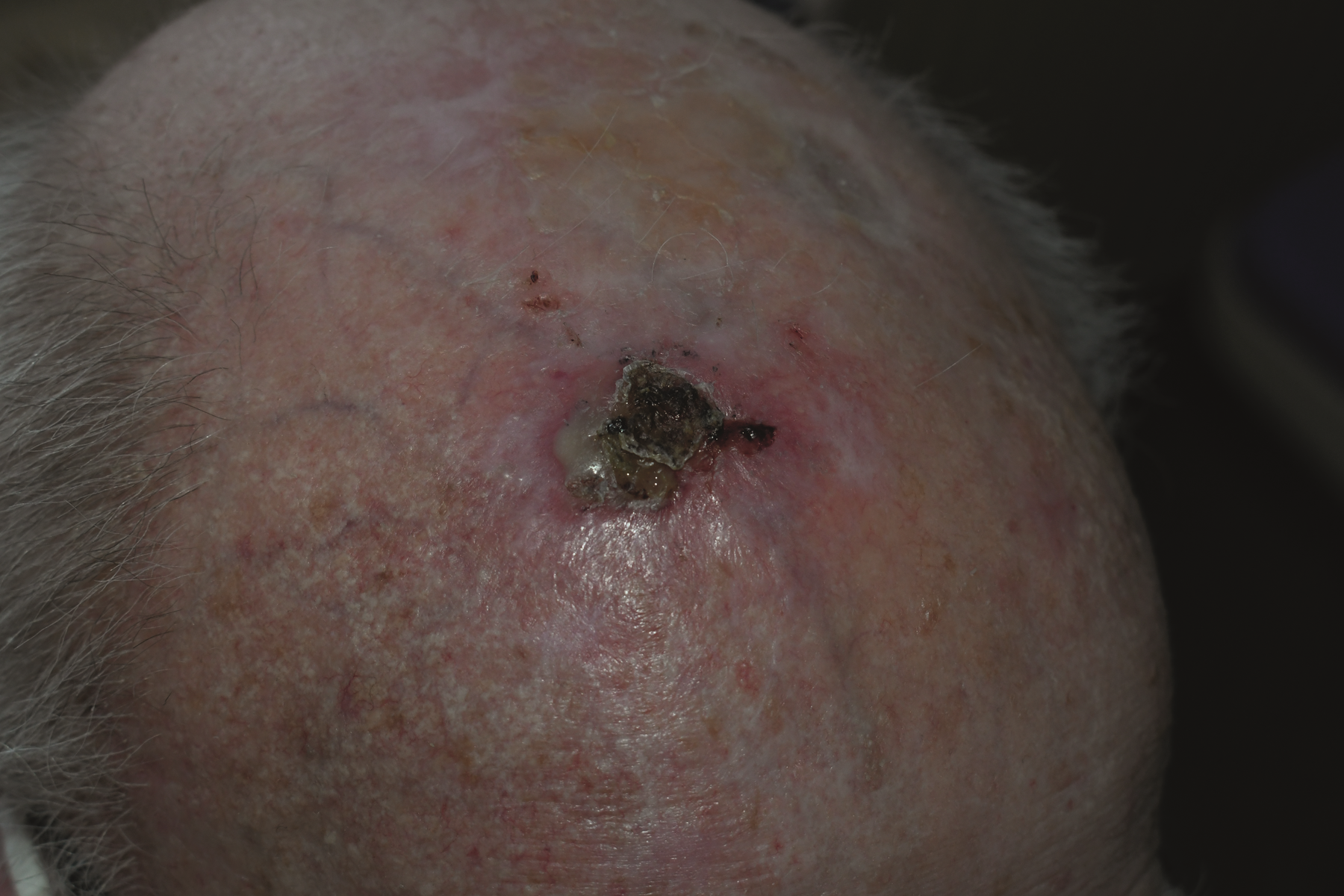
Squamous Cell Carcinoma
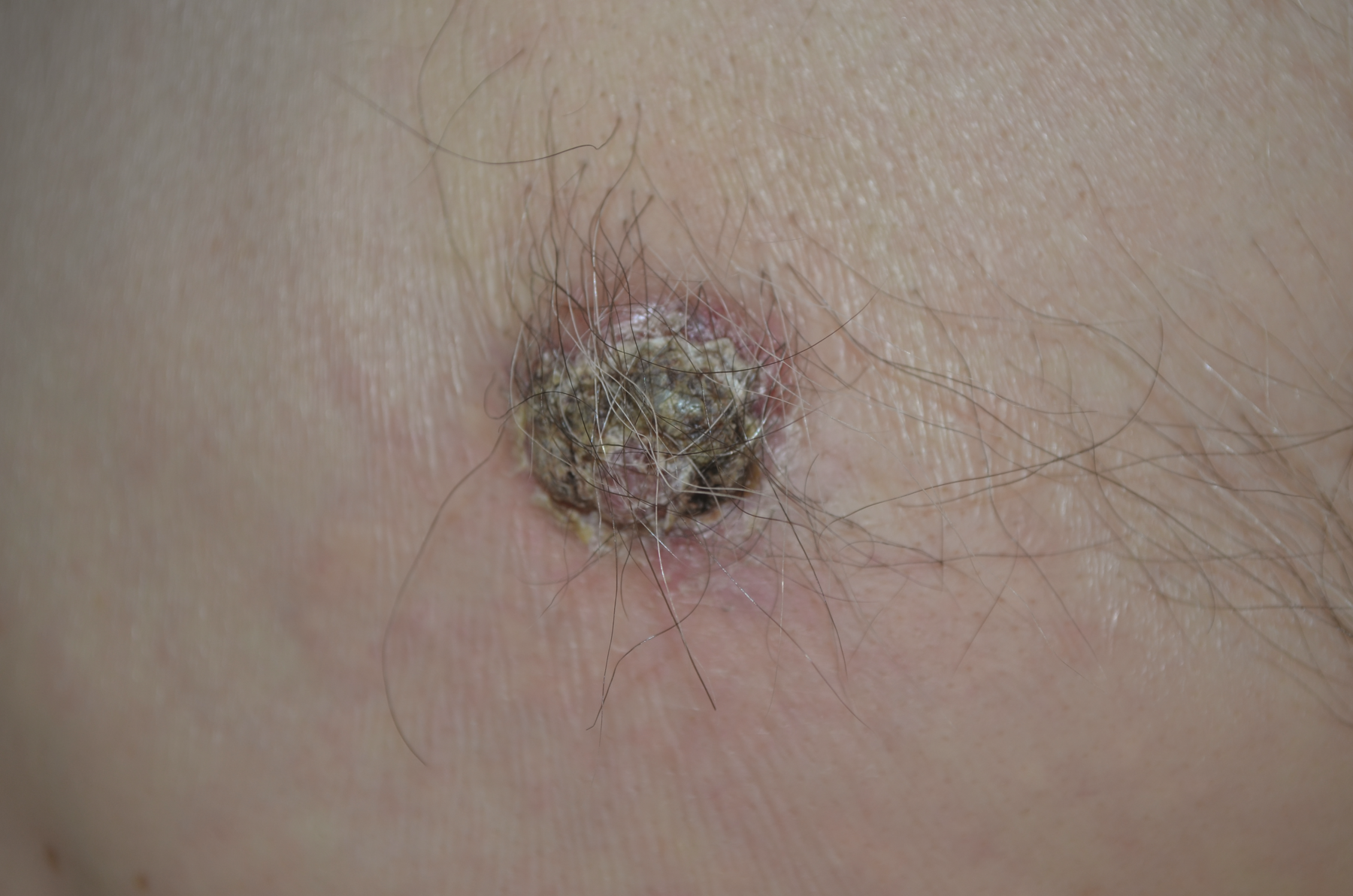
Basal Cell Carcinoma
Malignant Wounds can generate excessive suffering for the patient and their caregivers due to:3
- Malodour
- Excessive bleeding
- Pain
- Highly exudating
- Often disfiguring
Patients and their caregivers/families often require psychological, spiritual and emotional support along with physical care. The aim of malignant wound management is to reduce the devastating impact the wound has on the individual, their family and their care team, whilst acknowledging the potential for new wounds to develop as the carcinoma escalates or pressure injury/ulcers develop as the skin fails.1
How to assess a malignant wound
➔ Conduct a holistic patient assessment with a focus on patient quality of life, social and family support/environment.
➔ Conduct a wound assessment using a validated assessment tool, with the following special considerations:
- Watch for tunnelling or undermining.
- Assess odour, from the patient’s perspective, which can be caused by infection, necrotic tissue or exudate.
- Amount and type of exudate.
- Percentage of devitalised tissue.
- State of surrounding skin.
- Watch for bleeding and potential for haemorrhage.
- Effects of location (obstruction of airways, near major arteries, restriction of movement, restriction of eating or basic body functions, etc.).
Conduct a pain assessment and complete physical exam
➔ Conduct a detailed pain assessment to determine the nature and type of pain, duration, severity and impact of daily living, etc. using a validated pain assessment tool.
➔ Include a complete physical exam to check for other injuries/complications (i.e. pressure injuries, skin failure, etc.), including a nutritional assessment as patients with malignant fungating wounds often have significant problems with appetite due to odour.
Remember
ALWAYS take the patient’s goals of care into account. With fungating malignant wounds, patient and caregiver’s primary concerns may not be wound treatment but other issues such as odour, pain and mobility restrictions/activities of living.
➔ Examples of patient care goals
- Be able to visit with family and friends (i.e. clarity of thought and odour control).
- Live to see birth of grandchild (life extension).
- Being able to attend a family wedding (mobility).
- No pain.
- Etc.
Keep in mind
1. Schedule regular holistic patient and wound reassessments based on the patient’s changing condition and situation.
- Malignant wounds can expand and deteriorate rapidly and require frequent re-evaluation.4
- Complete a full body re-assessment to identify new wounds that may develop, except in the case of advanced end-of-life stages where it may not be appropriate to disturb the patient.
- The needs of the patient, overall health and patient and family care goals may also change rapidly over the course of treatment and need to be reviewed at each re-assessment.
- Amending actions taken and reprioritising the care model may be necessary on multiple occasions, as the patient becomes weaker and less able to care for themselves.
2. All treatments should be patient driven. It is also important to ask the patient’s permission at each visit before conducting assessments, change dressings etc.
How to develop a treatment and care plan
➔ Management of malignant wounds is complex and requires a multidisciplinary approach to care.
➔ Putting together a multidisciplinary/integrated care team is critical.
➔ The patient and their family/caregivers must be considered full and active members of the care team.
➔ The team should include everyone with a role in the patient’s clinical, psychological and spiritual care.
Keep in mind
When putting together a multidisciplinary care team, flexibility is key. Additional team members may be required as the patient progresses and new specialised skills are needed, i.e. pain management specialist, hospice care, etc.
➔ Developing treatment goals
- Achieving realistic, patient and family-centred measurable goals are the cornerstone of effective care.5
- Treatment goals must be patient driven, help alleviate social isolation and manage pain. It is critical that clinicians ask the patient before undertaking any treatment or assessment and respect the patient’s decision-making.
- Patient and family centered care (PFCC) is increasingly linked to improved communication, care quality, and patient decision making.6
- Patient centred care involves understanding the patient as a person, the patient-healthcare professional relationship, and coordination of care across the healthcare system.7
➔ SMART goals

SMART goals
➔ Treatment planning
- The treatment plan must be in keeping with the care goals of the patient and their family, which may change over time.4
- Overall goals should include patient comfort, confidence and sense of wellbeing, prevent social isolation and maintain or improve overall QoL.8
- Pain management is a critical part of the treatment planning. If pain is not being adequately managed refer.
- Patient reported pain can include pain due to the underlying condition and specific pain related to the wound site.
- It is important that a distinction be made between pain caused by stimulation of nerve endings (nociceptive pain), pain caused by nerve dysfunction (neuropathic pain) and pain caused by treatments or dressing changes as they all require different treatments.2,9
- Pain experienced during dressing changes can be mitigated by advising patients to take their oral medications 45 minutes prior to the nursing visit to ensure the pain medication is at full strength prior to any wound care treatments, or by using a “booster” dose of analgesia prior to treatment. Some studies have also demonstrated a positive effect from the use of topical opioids applied directly to the wound bed.2
- A pain specialist can help tailor the care to suit the evolving needs of the patient.2,4,10
- Pruritus or itchy skin can be a side effect of the tumour or of the treatment. Moisturisers, use of neutral soaps, topical anesthetics, localised temperature control, cortisone and antihistamines may help.10
- Treatment and control of exudate, odour and bleeding are often of immediate importance to optimise patient quality of life.
- Malodour is recognised as having a major physical and psychological impact on patients and families/caregivers. Determining the cause of the malodour can help in developing a realistic management plan.11
- There are some reports of success using off-label treatments such as: charcoal dressings, administration of chlorophyll tablets, use of antibiotics, silver dressings, medical honey, sugar, green tea bags and NPWT palliative therapies.
- There is some agreement that metronidazole gel administered topically and the use of oral metronidazole can reduce odour.
- Other typical strategies to control odour include
- Use of aromatherapies (some scents may cause nausea for patients. A trial- and error approach to determining which if any scents help may be required).
- Keeping room well ventilated.
- Kitty litter under the bed.
-
- For all odour reducing dressings, follow manufacturers’ instructions closely to ensure the most effective outcomes.
➔ WHO Analgesic Ladder
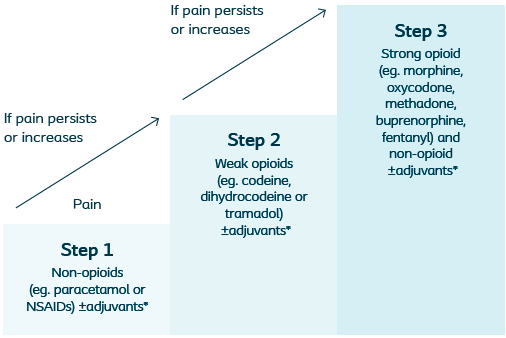
WHO Analgesic Ladder. *Adjuvants can be used along any step of the ladder, these may include antidepressants, anticonvulsants, corticosteroids and anxiolytics.
Keep in mind
1. Many treatments for these patients lack higher level evidence due to the nature of this patient population. Often a trial-and-error approach to reducing symptoms is required to find the solution that works best for the patient and family caregivers.
2. Patient and family/caregiver education is paramount. Understanding expected disease progression, effective supported self-care options and preparing for contingencies (i.e. haemorrhages) allow patients and families/carers to be actively and appropriately involved in treatment planning.
How to manage a malignant wound
➔ Cleansing & Debridement:
- Therapeutic cleansing/irrigation and debridement may be necessary to remove necrotic tissue and reduce odour.
- Self showering is a viable cleansing technique based on the patient’s abilities and preferences.
- Aggressive or sharp debridement is not recommended on malignant wounds. Autolytic debridement can be achieved using hydrating dressings or honey.5 Debulking tumours to remove necrotic tissue and reduce odour should only be done by a specialist.
- Mild wound cleansing is recommended to reduce the incidence of bleeding. Use of potable water, saline or mild antiseptic solutions at room or body temperature are recommended. Therapeutic irrigation and wound cleansing may not be appropriate if deep tunnelling is present.5
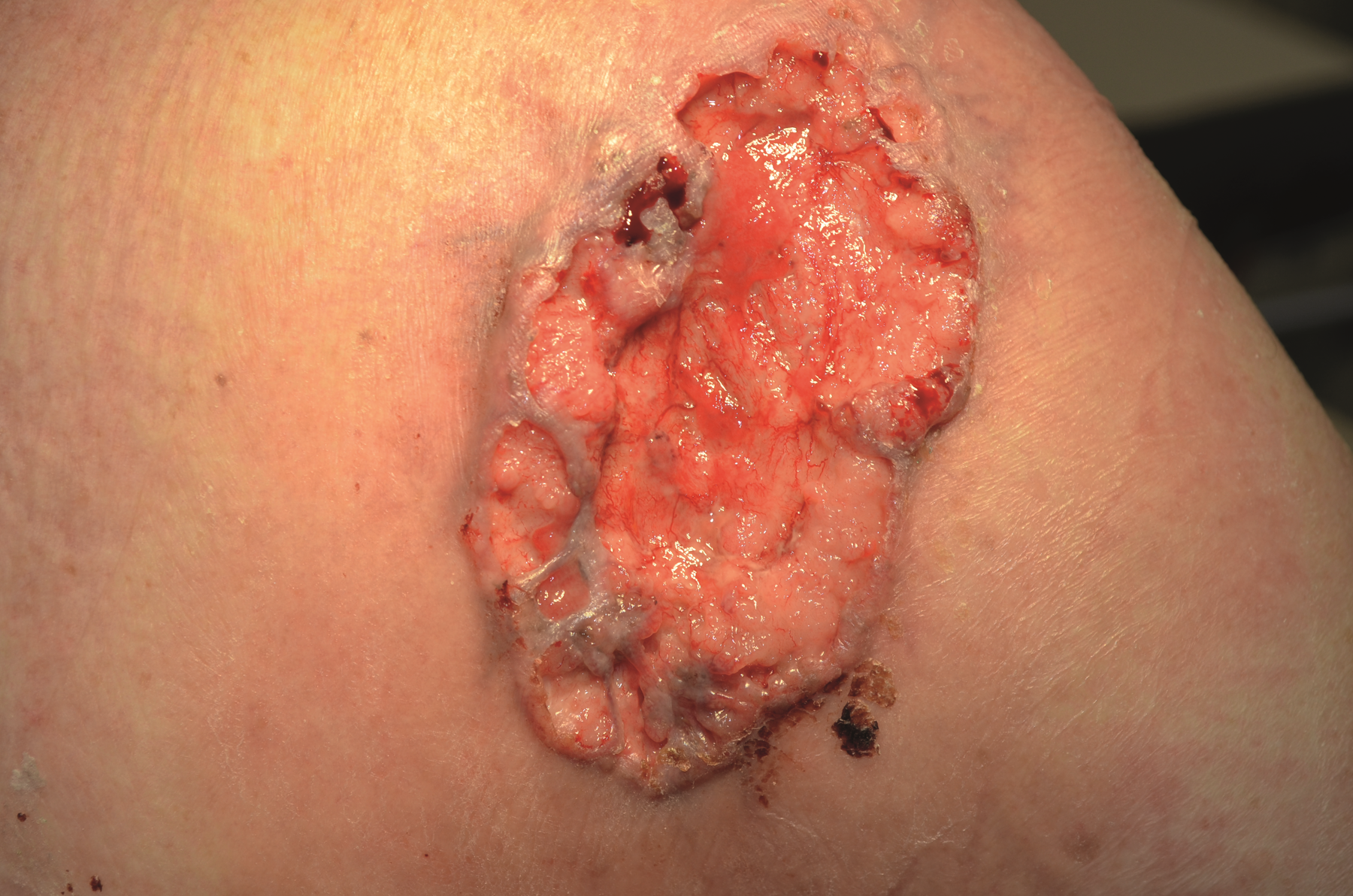
Basal Cell Carcinoma
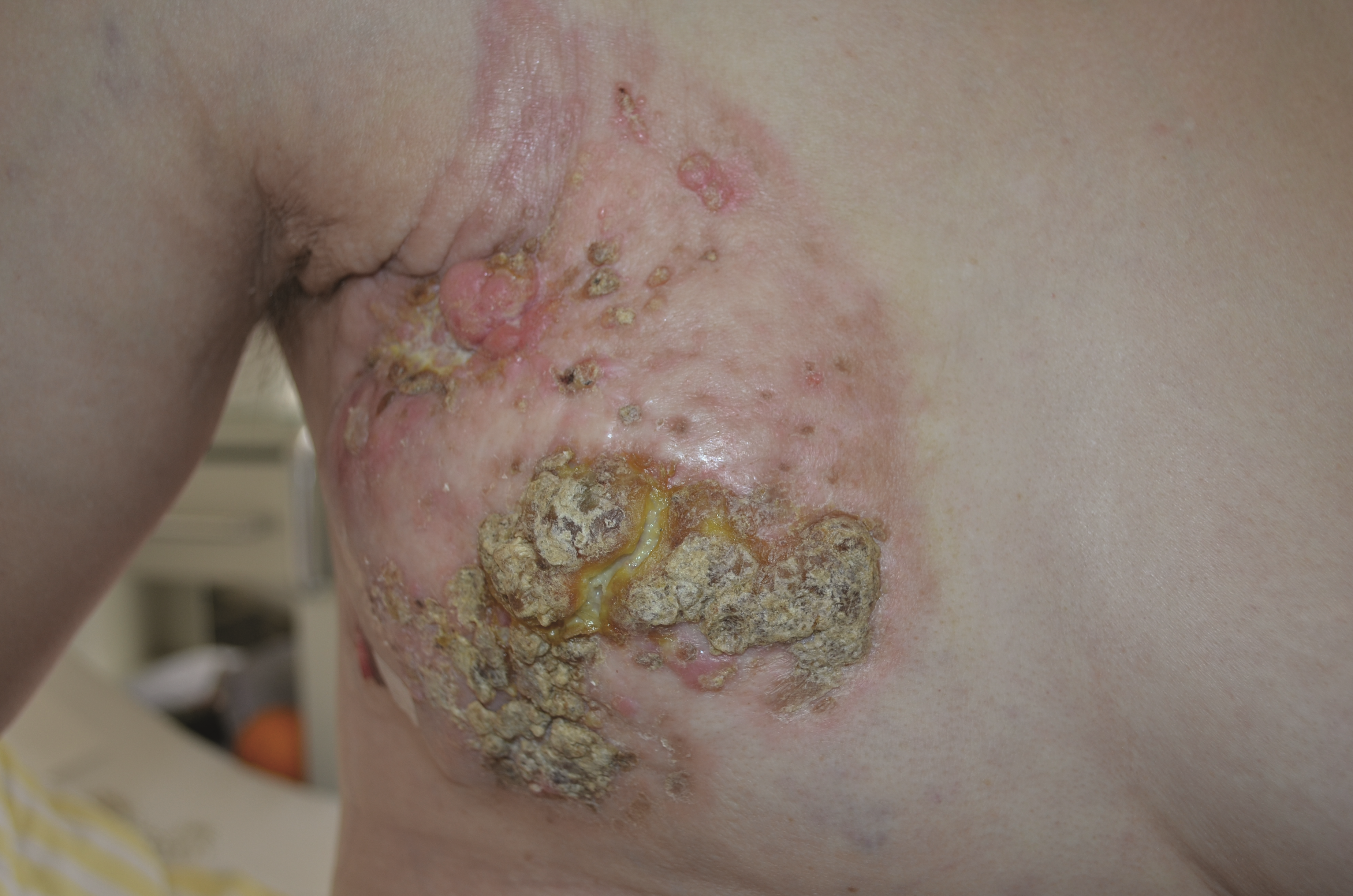
Breast carcinoma
Keep in mind
1. Decisions around therapeutic cleansing and debridement should always take into account patient comfort and care goals. Ask the patient if it is OK to cleanse the wound. If the patient declines, explain the benefits of the treatment, but if the patient does not want the treatment respect his/her wishes.
2. Avoid unnecessary manipulation of the wound, especially for patients with malignant end-of-life wounds
- Only swab if you are planning to treat for infection and where it is necessary to control bacteria where resistant organisms require special infection control measurements.12
- Controlling bacteria can decrease exudate, pain and odour and help stabilise a non healing wound.13
- If unexpected infection is persistent, spreading or if systemic infection is suspected refer.
Keep in mind
Localised inflammatory effects of the malignant wound may have many of the same characteristics as infection, such as appearing red, inflamed and warm to the touch.
How to choose dressing and additional therapy
➔ Dressing choice should always take into account current treatment and procedures that may impact dressing type and change frequency, such as radiotherapy.
➔ A dressing should manage exudate, prevent infection, protect periwound skin, allow the patient maximum mobility, comfort and security and be non-traumatic on application and removal.
➔ Non-adherent soft silicone dressings have been shown to cause less pain upon removal.2
➔ Choose a dressing that:
- Is comfortable and allows patient maximum mobility.
- Is convenient for patient and caregiver.
- Has a long wear time, to reduce painful dressing changes.
- Is non traumatic on application and removal.Absorbs excess exudate, bleeding and protects periwound skin.
• Reduces infection risk and odour.
➔ Avoid the use of petroleum impregnated dressings and occlusive hydrocolloid dressings in fungating wounds.5
Remember
1. It is important to ask the patient’s permission at each visit before conducting a dressing change.
2. Avoid MARSI by using non-adhesive dressings and careful dressing removal.
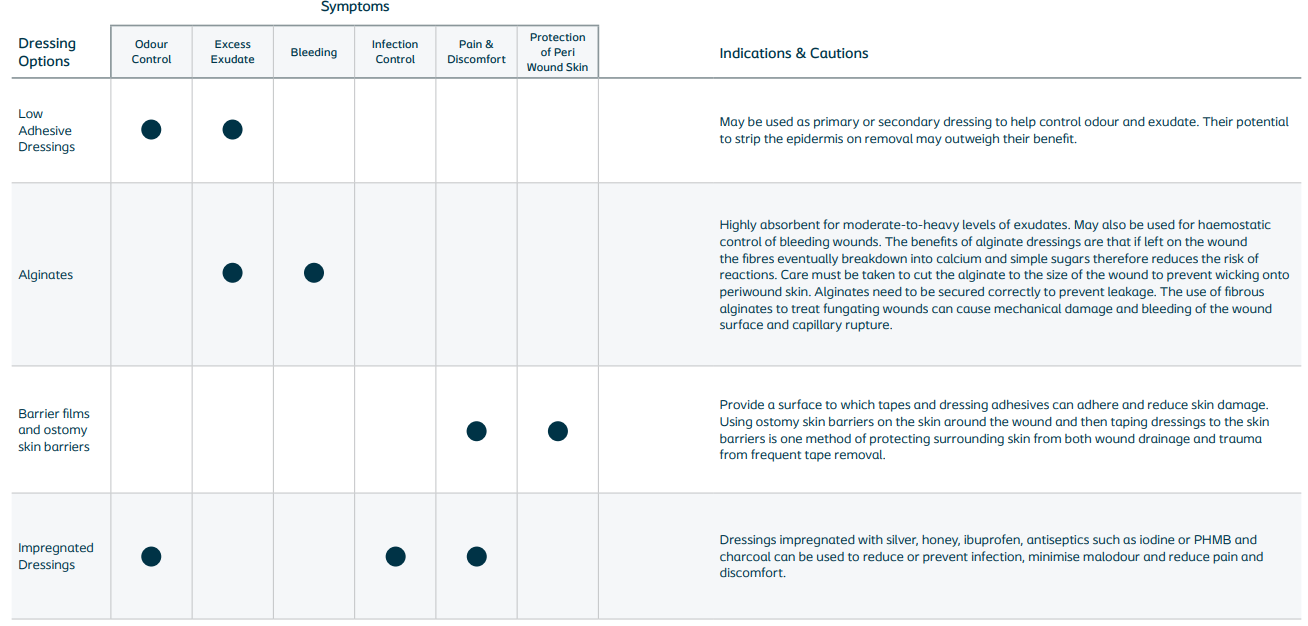
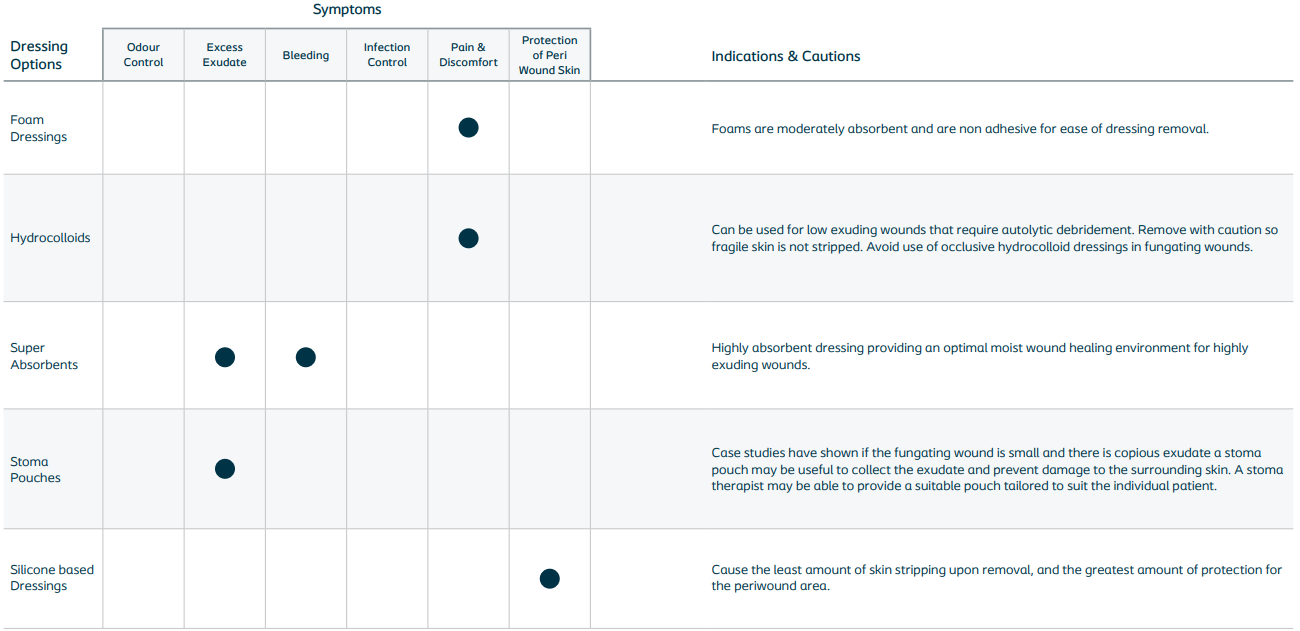
➔ Malignant wounds are often highly exudating and irregular in size and shape, which makes them difficult to dress and may require an unorthodox approach. A multiple layered dressing approach may be required. Dressing selection should be based on patient needs and preferences and local policy/protocol/formularies. The following chart (see below) breaks down some of the basic theory around dressing types and how they can help manage symptoms for patients with malignant fungating wounds.
Be aware
If patient is not responding to standard care, consider referral for adjunct therapies such as:
- Surgery
- Radiotherapy
- Hormone therapy
- Electrochemotherapy (TENS)
- Laser therapy
- Chemotherapy
Dressing options for different symptoms
Monitor patient's progress towards care goals
➔ Care must be flexible and focused on the patient’s priorities, as well as management and control of symptoms.
➔ Assess progress towards care goals and acknowledge that the patient’s goals may change as their condition progresses.
➔ Taking photos of the wound at dressing changes can help assess progression and will allow other members of the care team to “see the wound” without disturbing the patient. Always ask patient permission before taking the photo and also ask patient if they would like to see the image.
➔ Monitor environment of care and openly discuss care options with patient and family/caregivers.
Remember
The patient should ALWAYS drive decision-making.
➔ Patient and care giver education and communication:
- Malignant wound care must always focus on the needs and wishes of the patient.
- Continuous open communication between all members of the multidisciplinary team, the patient and the patient’s family/caregivers is crucial to ensure effective coordinated care and to manage expectations.
- Clinical and psychological support for the patient and their family/ caregivers should be part of every interaction with the patient.
- Preparing the patient and family/caregivers for future stages of care is important (i.e. if wound is near a major artery and there is a possibility of a large or fatal bleed, suggest keeping dark towels on hand to decrease the stress and anxiety from the sight of blood).
- Providing written instructions to patients and families will often help with information retention.
- Connecting patients and family/caregivers to community resources can often assist in education and communication efforts and offer additional support.
➔ Caregiver support
- Clinicians who treat patients with malignant wounds and end-of-lifewounds often face complex challenges of care and additional factors such as moral distress, burnout, compassion fatigue and death anxiety.14
- Clinician self-care should be prioritised and include extended supervision, reflective practice, access to on-the-spot debriefs, and other support services.
- Patients found that they felt isolated and cut off by nurses who struggled to acknowledge their own distress.8

When to refer or contact a specialist
- If pain is not adequately controlled.
- If unexpected infection is spreading or not adequately controlled.
- When alternative therapies, debulking or sharp debridement are necessary.
- If episodes of brisk hemorrhage, or uncontrolled bleeding occur.
- If bone or organs become exposed. Sudden changes in overall health or condition, beyond the expected patient trajectory.
- For adjunct therapies, such as palliative radiation.
Glossary of malignant wound terms
Malignant Wound
– A cancerous lesion involving the skin, which is open and may be draining. The lesion may be a result of a primary cancer, or a metastasis to the skin from local spread or local invasion. It may take the form of a cavity, an open area on the surface of the skin, skin nodules, or a nodular growth extending from the surface of the skin.12
End-Of-Life
– Sibbald (2009)15 defines end of life as a phase of life when a person is living with an illness that will often deteriorate and eventually cause death.
Fungating Wound
– when a tumour that is growing under the skin breaks through the skin’s surface and creates a wound. As the cancer grows, it can block and damage blood vessels, reducing oxygen supply to the surrounding skin and tissue causing necrosis.
Kennedy Terminal Ulcer (KTU)
– an unavoidable skin breakdown which occurs in some patients as part of the dying process.
MARSI
– Medical Adhesive Related Skin Injury most often caused by the use of adhesives or the aggressive removal of dressings.
Marjolin’s Ulcer
– a cutaneous malignancy that forms in the area of previously injured skin, burn scars, and chronic wounds.
Pruritus
– refers to itchy skin and can have cutaneous, neuropathic, neurogenic, or psychogenic origins.
Tunnelling and Undermining
– when passages or openings develop under or adjacent to the wound bed or there is erosion under the wound edges. Both tunnelling and undermining create cavities within the wound bed where exudate can pool and cause infection.
For a glossary of general wound care terms consult The Wound Care Pathway:

