Get full access with a free account
Benefits of the Coloplast® Professional Educational platform
- Get full access to all educational content, events and resources
- Track your progress
- Share content with your collegues
- Share supporting material with your patient
Biofilm and its role in wound infection
In this section, you will learn about:
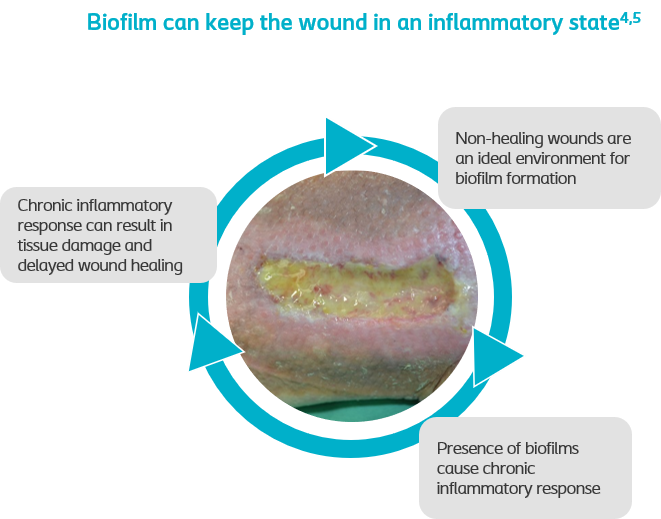
How do biofilm affect wound healing?
are probably the most important single cause of persistent, delayed healing in wounds.2 As figure 1 illustrates, they are also thought to delay wound healing by effecting an inappropriate inflammatory response, which is ineffective, poorly orchestrated and damaging to host tissues.2
There is increasing evidence that biofilm are present in most, if not all, chronic, non-healing wounds.3 Therefore, if you diagnose that your patient has an infection in a chronic wound, it’s recommended that you follow the guidelines for preventing and managing biofilm.2
Two types of bacteria formations
Bacteria are often viewed as being single cells that multiply rapidly when in exponential growth. This is referred to as ‘planktonic form’ and relates mostly to acute infections. Bacteria can also form aggregates, or communities, of slow-growing cells – this kind of formation is referred to as ‘biofilm’. The most common biofilm formers are Staphylococcus aureus and Pseudomonas aeruginosa.2
How do you detect biofilm?
Detecting biofilm can be challenging, due to the following factors:
- Biofilm are microscopic structures, which are invisible to the naked eye. So you need to use a high-powered microscope to detect them.
- In a clinical setting, the best detection method is a tissue biopsy. However, biofilm are small and unequally distributed in the wound bed. A wound may have different species of biofilm, and they are typically scattered around in small, isolated, single-species islands. That’s why they can be easy to miss.
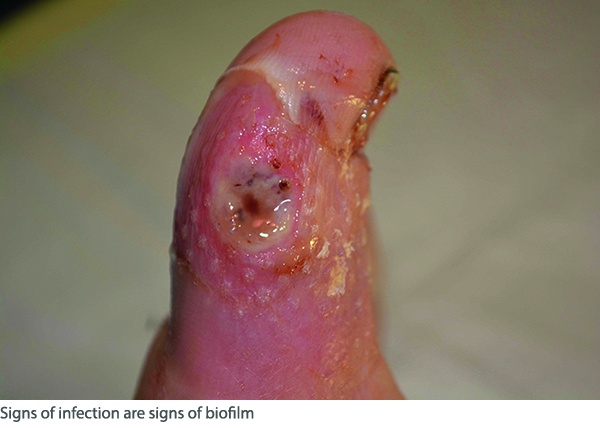
Signs of wound infection
Given the expense and time involved in tissue biopsy and microscopy, most clinicians diagnose biofilm by identifying the common signs of wound infection. Some of these signs are:2,4
- sloughy tissue
- increased levels of exudate
- poor granulation / friable hyper granulation
- malodour
- delayed healing
If a wound still shows these signs of infection after it has been managed correctly and the patient has received appropriate health support, biofilm may be present.
When should you suspect biofilm?
Try asking yourself the following questions:2
- Have all appropriate diagnostic and therapeutic measures been followed?
- Is the wound failing to heal as expected?
- Does the wound show signs of local infection or inflammation?
If you answer ‘Yes’ to at least 2 of these questions, it would be clinically relevant to treat for biofilm.
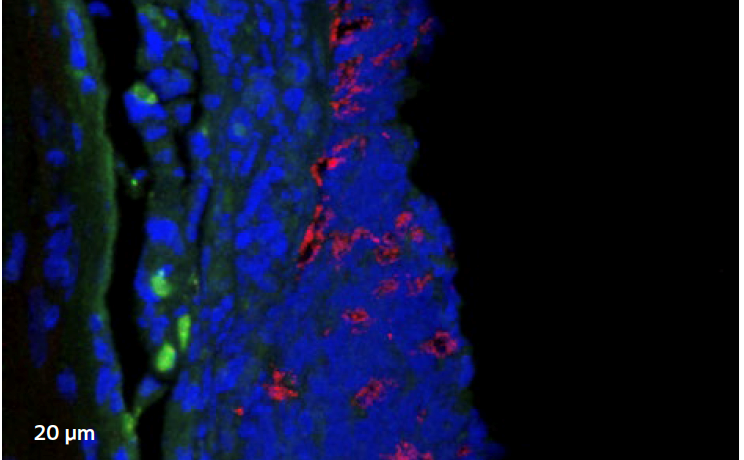
Confocal laser scanning microscopy (CLSM)
Image 1 shows a microscopic image of biofilm (highlighted in red), with clusters often less than 1/10 mm. This results in many swabs coming back inconclusive.
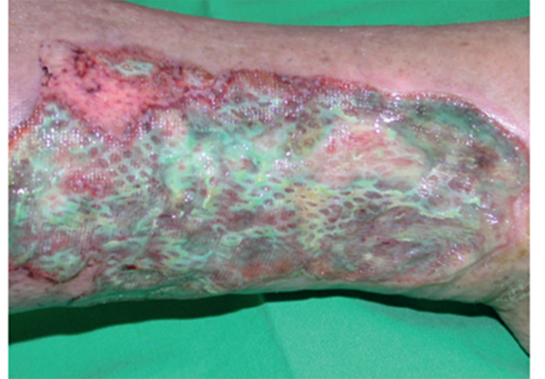
Example of wound with suspected biofilm
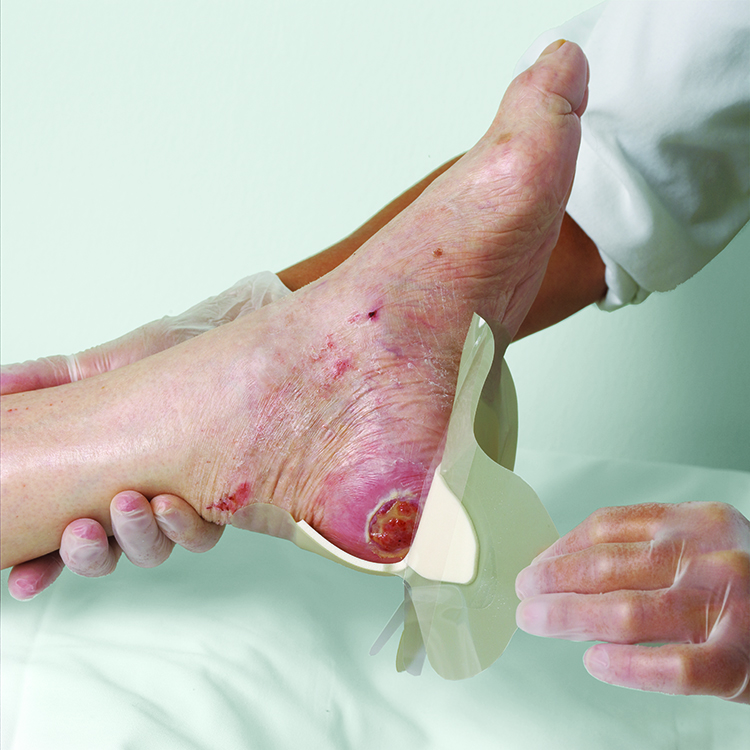
You should suspect biofilm in ‘healable’ wounds, that are non-healing, if you have taken all of the appropriate measures.1
How to manage biofilm effectively
combination of methods to disrupt and decrease biofilm and prevent it from reforming.
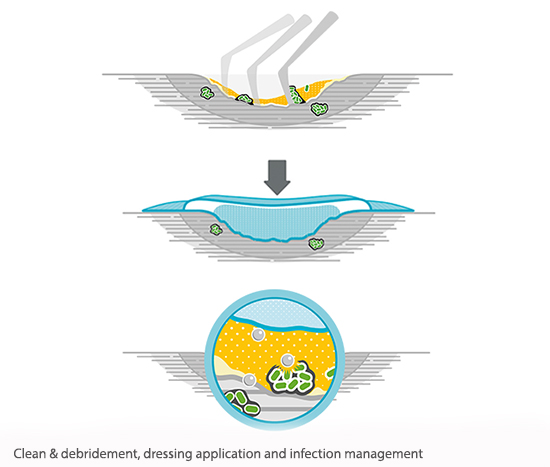
To effectively manage biofilm, the IWII 2016 consensus document recommends the following three steps:4
- Therapeutic cleansing at every dressing change, and ongoing aseptic management
- Conservative sharp and mechanical debridement, e.g. a curette
- Thorough cleansing and care after debridement
Another publication recommends using antimicrobial dressings. This is a clean and cover’ approach. By using these dressings between debridement, you reduce the planktonic bacteria’s ability to re-establish a biofilm. You also protect the wound from contamination by other microbes.2
For more information on preventing and managing biofilm, go to the section on How to prevent and manage biofilm.
References
- Swanson, Terry. Keast, David. Bain, Kimberly & Mark. Preventing and treating infection in wounds: translating evidence and recommendations into practice. Wounds International 2020. Vol 11, issue 4
- Keast, David & Swanson, Terry. White paper – A practical summary for the management of wound infections and biofilm, Coloplast 2020
- Dowsett C et al. A focus on the Triangle of Wound Assessment – addressing the gap challenge and identifying suspected biofilm in clinical practice. Wounds International 2019:10 (3)
- International Wound Infection Institute (IWII) Wound infection in clinical practice. Wounds International 2016.
You may also be interested in…

Triangle of Wound Assessment
Conduct a holistic and systematic wound assessment with our tool.